Pelvic Exams: A Complete Guide on What to Expect and How to Prepare
 Apr, 4 2026
Apr, 4 2026
Key Takeaways for Your Visit
- The exam typically lasts 10-15 minutes and focuses on the vulva, vagina, cervix, and uterus.
- Preparation is minimal, but tracking your cycle and avoiding douches helps get accurate results.
- You have the right to ask for a chaperone, request a specific speculum size, or stop the exam at any time.
- Common screenings like Pap tests are often bundled into the same appointment.
What Exactly is a Pelvic Exam?
At its core, a pelvic exam is a physical examination of the female reproductive organs to check for abnormalities and screen for diseases. It isn't just one single check; it's a series of steps designed to give your provider a full picture of your pelvic health. While many associate it strictly with the Pap smear, that is actually just one part of the larger process.
Your healthcare provider-usually a Gynecologist or a Nurse Practitioner-will look at the external and internal structures. They are checking for things like cysts, fibroids, or signs of infection. If you're experiencing pelvic pain or irregular bleeding, this exam is where they find the physical evidence needed to make a diagnosis.
The Step-by-Step Process: What Happens During the Visit
The exam follows a predictable pattern. Understanding the sequence helps you manage the physical sensations and reduces the "surprise" factor.
- The Visual Inspection: The provider starts by looking at the Vulva. They check for redness, sores, or unusual discharge. This is a non-invasive step where they are simply observing the external skin and openings.
- Speculum Insertion: This is the part most people dread. The provider uses a Speculum-a tool made of plastic or metal-to gently open the vaginal walls. This allows them to see the Cervix clearly. You'll feel a sensation of pressure and stretching, but it shouldn't be sharp pain.
- The Screening (Pap Test): Once the cervix is visible, they use a small brush or spatula to collect cells. This is the Pap smear, which screens for Human Papillomavirus (HPV) and precancerous changes. It feels like a quick pinch or a scratch.
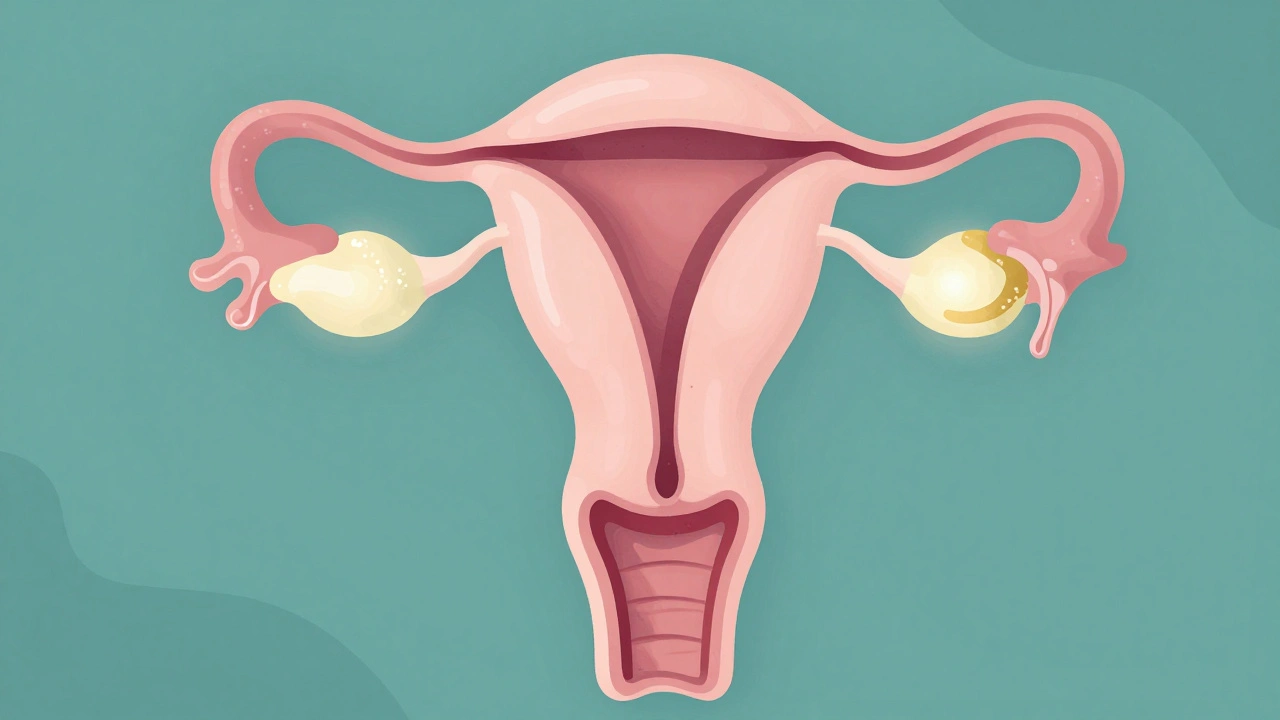
- Bimanual Examination: After removing the speculum, the provider inserts two gloved fingers into the vagina while pressing down on your lower abdomen with their other hand. This "sandwich" technique allows them to feel the size and shape of the Uterus and Ovaries. This is crucial for detecting ovarian cysts or uterine fibroids.
How to Prepare for Your Appointment
You don't need to undergo a rigorous ritual to get ready, but a few simple choices can make the results more accurate and your experience more comfortable.
First, timing is everything. If possible, schedule your exam for a time when you aren't on your period. While providers can still perform exams during menstruation, heavy bleeding can sometimes obscure the view of the cervix or interfere with the cell samples in a Pap test. If you're unsure, a quick call to the office can confirm if they prefer you to wait.
Avoid using douches, scented soaps, or vaginal creams for at least 48 hours before the visit. These products can alter the pH balance or leave residues that make it harder for the lab to analyze samples. Think of it like a clean slate; the more "natural" the environment, the clearer the data.
Clothing choice also matters. Wearing a skirt or a loose dress can make the transition to the exam table faster, though the clinic will always provide a gown. More importantly, write down your questions. When the gown goes on, it's easy to forget that you wanted to ask about a specific change in your cycle or a new symptom you've noticed.
| Factor | Do This | Avoid This |
|---|---|---|
| Timing | Schedule mid-cycle | Scheduling during heavy flow |
| Hygiene | Gentle external wash | Internal douching or creams |
| Clothing | Loose-fitting clothes | Complex multi-layered outfits |
| Communication | List of symptoms/dates | Relying on memory during the exam |
Managing Anxiety and Discomfort
Physical discomfort is often amplified by mental tension. When you tense your pelvic floor muscles, the speculum feels tighter and the exam takes longer. The goal is to create a feedback loop of relaxation.
Try the "belly breath." Instead of taking shallow chest breaths, breathe deep into your stomach. This naturally relaxes the pelvic muscles and helps you ride out the pressure. If you feel a sharp pain, don't "tough it out." Tell your provider immediately. They can adjust the angle of the speculum or use a smaller size to make it bearable.
You also have agency over the environment. If you feel nervous, ask for a medical chaperone-usually a nurse-to be in the room. If you've had a bad experience in the past, tell the provider before they begin. A simple statement like, "I'm very anxious about this part," allows them to slow down and explain each movement before it happens.

Understanding Your Results
After the exam, you won't usually get answers immediately because the samples are sent to a lab. However, the bimanual exam provides instant feedback. Your doctor might tell you right then if your uterus feels "tipped" or if they felt a small cyst on an ovary.
For the lab work, a "normal" Pap result means no precancerous or cancerous cells were found. If a result comes back as "ASC-US" (Atypical Squamous Cells of Undetermined Significance), don't panic. This is a very common result and often just means there is some inflammation or a minor infection that needs treating, not necessarily cancer.
Does a pelvic exam always include a Pap smear?
Not necessarily. A pelvic exam is the physical check of the organs, while a Pap smear is the specific act of collecting cells from the cervix. Depending on your age and health history, you might have a pelvic exam for pain or check-ups without needing a Pap smear every single time.
How often should I actually get these exams?
Guidelines vary, but generally, most women start screening at 21. For those with a normal history, a Pap test every 3 to 5 years is common. However, a general pelvic exam annually is often recommended to monitor overall reproductive health and discuss any new symptoms.
What should I do if the exam is too painful?
Immediately tell your provider to stop or adjust. You can ask for a smaller speculum, suggest using more lubricant, or even request a different position. If you have a condition like vaginismus, mention this beforehand so they can use specialized techniques.
Is it normal to bleed a little after the exam?
Yes, light spotting is common after a Pap smear because the cervix is very sensitive and the brush can cause minor irritation. If the bleeding is heavy or accompanied by severe pain, you should contact your clinic.
Can I request a female provider?
Absolutely. You have the right to feel safe and comfortable. When booking your appointment, simply request a provider whose gender you are comfortable with. Most clinics are very accommodating to these requests.
Next Steps and Troubleshooting
Once you leave the office, the process isn't quite over. Keep an eye on your patient portal or wait for the phone call regarding your lab results. If you don't hear anything within two weeks, it's perfectly acceptable to call the office and ask for your results. Sometimes things get lost in the shuffle, and being your own advocate ensures nothing is missed.
If you find that pelvic exams are consistently traumatic or physically impossible due to pain, talk to your doctor about "trauma-informed care." There are ways to modify the exam, such as using a different speculum or focusing on a less invasive approach to screening. Your mental well-being is just as important as the physical results of the test.